 Hard exudates are 500 µm or less (1/3 DD) from the center of the macula with thickening of adjacent retinal tissue.Thickening of the retina is 500 µm or less (1/3 DD) from the center of the macula.1-4 It is considered clinically significant macular edema (CSME) if one of the conditions below is met. Patients with diabetic macular edema (DME) exhibit retinal thickening within 2 disc diameters (DDs) of the center of the macula. Send a detailed report to the patient’s PCP and/or endocrinologist so that they are aware of the findings, which will aid their decision making on treatment. Encourage them to monitor their blood sugar and diet. It is important to discuss findings with patients, especially those who were recently diagnosed with diabetes, to ensure that they understand that MAs indicate early end organ damage from their disease and that they are educated on its possible ramifications. Patients with mild NPDR do not need to be referred to a retina specialist unless you are concerned about or have confirmed a diagnosis of DME (see The 411 on DME). Use fundus photography, if available, for easier future comparison. Documenting subtle findings and noting their exact locations will help you to monitor patients for disease progression. 2 If one or more MAs are present in the eye of a patient not yet diagnosed with diabetes, he or she should be considered a diabetes suspect and should see his or her PCP for further testing. 2 There is a 5% risk that mild NPDR will progress to PDR within 1 year. 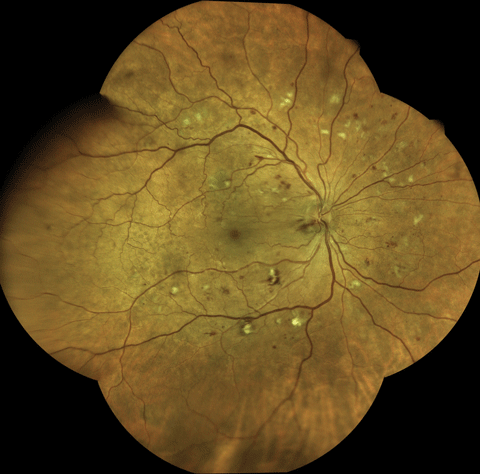
These patients should have a dilated eye examination every 12 months. Note the hemorrhage within the inferior arcades. This patient with type 2 diabetes has mild NPDR without macular edema. 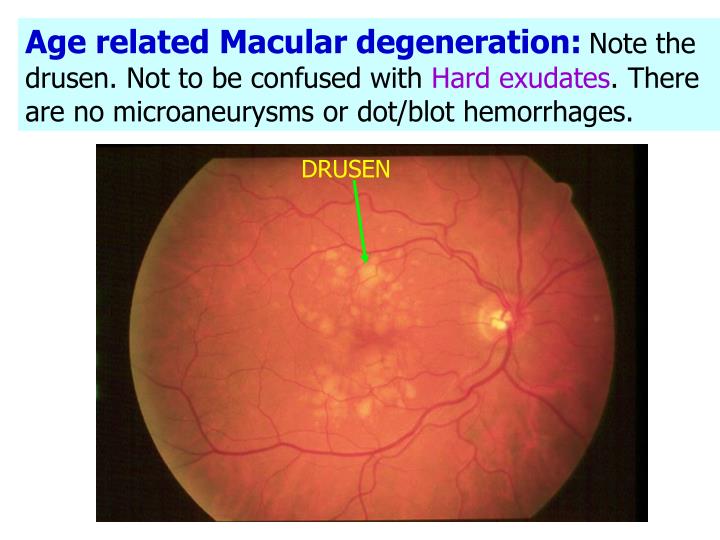
This article provides tips on caring for patients with diabetes, including advice calibrated to the specific stages of diabetic retinopathy (Table).įigure 1. 2,4 Women who were previously diagnosed with type 1 or 2 diabetes should have a comprehensive dilated eye examination before becoming pregnant or within the first trimester. 2,4 Patients with type 2 diabetes should receive a comprehensive dilated eye examination at the time of diagnosis and yearly thereafter. The American Optometric Association’s Practice Guidelines and the American Diabetes Association both state that patients with type 1 diabetes should have a comprehensive dilated eye examination within 5 years of disease onset. This explains the importance of monitoring all patients with diabetes and working with primary care physicians (PCPs) or endocrinologists to help manage these patients. 3Īs an optometrist, you treat and observe the only place in the human body where physical damage to blood vessels caused by systemic diseases can be viewed noninvasively. 1,2 These studies also found that the incidence of proliferative diabetic retinopathy (PDR) varied from 2% in those who had diabetes for less than 5 years to 15.5% in those who had diabetes for 15 or more years.  
Researchers have found that nonproliferative diabetic retinopathy (NPDR) was present in 25% of patients 5 years after they were diagnosed with diabetes, 60% at 10 years, and 80% at 15 years. Patients with either type 1 or type 2 diabetes are at risk of developing neurovascular complications that can lead to diabetic retinopathy and/or diabetic macular edema (DME). Patients with severe NPDR have a 52% risk of developing PDR within 1 year, are at a high risk of disease progression and permanent vision loss, and are most likely experiencing neuropathy elsewhere.Patients with moderate NPDR have a 12% to 27% risk of developing PDR within 1 year and should be seen every 6 to 8 months.Patients with mild NPDR do not need to be referred to a retina specialist unless you are concerned about or have confirmed a diagnosis of DME. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |



 RSS Feed
RSS Feed
